|
 |
- Search
| J Neurointensive Care > Volume 4(1); 2021 > Article |
|
Abstract
Objective
Methods
Results
Acknowledgements
Fig.┬Ā2.

Table┬Ā1.
| Characteristics | Mild (n=61) | Moderate (n=28) | Severe (n=12) | p-value |
|---|---|---|---|---|
| Sex (Male:Female) (%) | 3.7 : 1 | 2.2 : 1 | 5:1 | 0.0435 |
| Age ┬▒ | 56.4 (┬▒12.4) | 59.9 (┬▒11.7) | 59.4 (┬▒17.6) | 0.4441 |
| Admission | ||||
| ŌĆāsBP ┬▒ | 170.5 (┬▒42.0) | 170.7 (┬▒31.2) | 176.3 (┬▒35.0) | 0.9128 |
| ŌĆādBP ┬▒ | 100.0 (┬▒27.5) | 97.9 (┬▒27.4) | 101.0 (┬▒27.9) | 0.9376 |
| ŌĆāmBP ┬▒ | 123.5 (┬▒30.1) | 122.2 (┬▒25.3) | 126.1 (┬▒29.4) | 0.9380 |
| ŌĆāBST ┬▒ | 146.9 (┬▒52.2) | 183.9 (┬▒68.8) | 209.6 (┬▒74.5) | 0.0014 |
| Underlying ds. (%) | ||||
| ŌĆāHTN | 43 (70.5%) | 14 (50.0%) | 8 (66.7%) | 0.1685 |
| ŌĆāDM | 8 (13.1%) | 4 (14.3%) | 4 (33.3%) | 0.2110 |
| ŌĆāVascular lesion | 4 (6.6%) | 3 (10.7%) | 0 (0%) | 0.6154 |
| ŌĆāESRD | 4 (6.5%) | 4 (14.3%) | 1 (8.3%) | 0.4601 |
| ŌĆāCM | 9 (14.8%) | 2 (7.1%) | 0 (0%) | 0.3666 |
| ŌĆāMetastatic brain tumor | 2 (3.3%) | 0 (0%) | 0 (0%) | 1.0000 |
| Perviouscancer history | 10 (16.4%) | 4 (14.3%) | 0 (0%) | 0.3753 |
| Antiplatelets and anticoagulants use* | 6 (9.8%) | 5 (17.9%) | 3 (25%) | 0.2244 |
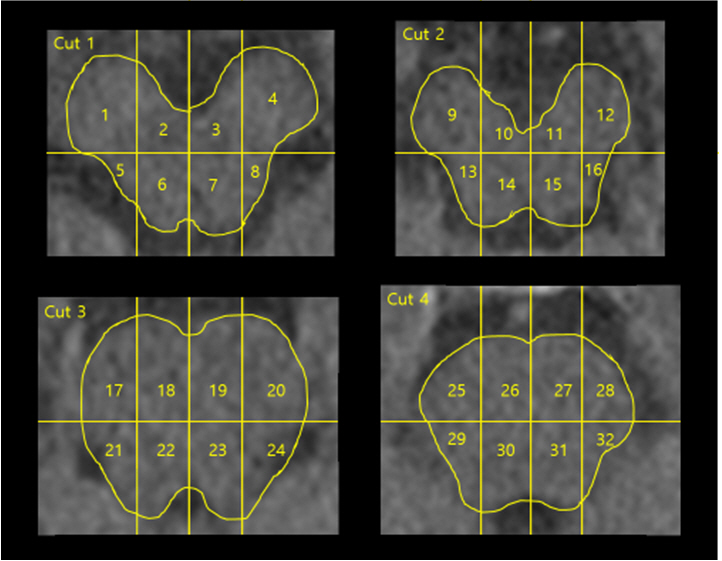
sBP: Systolic blood pressure, dBP: Diastolic blood pressure, mBP: Mean blood pressure, ds.: disease, HTN: Hypertension, DM: Diabetes mellitus, ESRD: End-stage renal disease, CM: Cavernous malformation, Hemorrhage volume: Mild, 1ŌĆō10 colored cells (0.5ŌĆō5 cm3), moderate: 11ŌĆō20 colored cells (5ŌĆō10 cm3), severe: 21ŌĆō32 colored cells (10ŌĆō15 cm3).
Table┬Ā2.
| Months | Mild (n=61) | Moderate (n=28) | Severe (n=12) | p-value | |
|---|---|---|---|---|---|
| GCS score ┬▒ | 0 | 11.36 (┬▒0.47) | 4.68 (┬▒0.69) | 3.08 (┬▒1.05) | < 0.0001* |
| 6 | 12.54 (┬▒0.41) | 6.16 (┬▒0.72) | < 0.0001** | ||
| 12 | 12.95 (┬▒0.39) | 7.02 (┬▒0.74) | < 0.0001** | ||
| 24 | 12.89 (┬▒0.55) | 7.31 (┬▒1.93) | 0.4547** | ||
| 0 vs. 24 | +1.53 (┬▒0.58) | +2.64 (┬▒1.94) | 0.0001* | ||
| ECOG ┬▒ | 0 | 2.54 (┬▒0.13) | 3.89 (┬▒0.19) | 4.00 (┬▒0.29) | < 0.0001* |
| 6 | 2.15 (┬▒0.14) | 3.63 (┬▒0.26) | < 0.0001** | ||
| 12 | 2.04 (┬▒0.14) | 3.63 (┬▒0.28) | 0.3482** | ||
| 24 | 2.05 (┬▒0.14) | 3.15 (┬▒0.30) | < 0.0001** | ||
| 0 vs. 24 | -0.49 (┬▒0.10) | +0.74 (┬▒0.26) | 0.6583* | ||
| mRS ┬▒ | 0 | 3.25 (┬▒0.21) | 4.93 (┬▒0.31) | 5.08 (┬▒0.48) | < 0.0001* |
| 6 | 3.15 (┬▒0.21) | 5.59 (┬▒0.32) | 6.00 (┬▒0.48) | < 0.0001** | |
| 12 | 2.93 (┬▒0.22) | 5.82 (┬▒0.41) | < 0.0001** | ||
| 24 | 2.82 (┬▒0.23) | 5.24 (┬▒0.56) | < 0.0001** | ||
| 0 vs. 24 | -0.43 (┬▒0.13) | 0.32 (┬▒0.49) | < 0.0001* |
Table┬Ā3.
| Hemorrhage volume | Months |
mRS ┬▒ |
p-value |
mRS ┬▒ |
p-value | ||
|---|---|---|---|---|---|---|---|
| Anterior | Posterior | Midbrain | Pontine | ||||
| Mild | 0 | 3.43 (┬▒0.44) | 3.21 (┬▒0.33) | 0.6512 | 1.67 (┬▒1.00) | 3.35 (┬▒0.23) | 0.1068 |
| (n=60)* | 6 | 3.38 (┬▒0.44) | 3.08 (┬▒0.33) | 0.6246* | 0.67 (┬▒1.25) | 3.27 (┬▒0.29) | 0.0548* |
| (n=59)* | 12 | 3.09 (┬▒0.46) | 2.91 (┬▒0.34) | 0.0277* | 0.67 (┬▒1.47) | 3.57 (┬▒0.35) | 0.0459* |
| 24 | 3.09 (┬▒0.46) | 2.73 (┬▒0.35) | 0.9288* | 0.67 (┬▒1.55) | 3.39 (┬▒0.46) | 0.4986* | |
| 0 vs. 24 | -0.34 (┬▒0.24) | -0.48 (┬▒0.18) | 0.4892 | -1.00 (┬▒1.04) | +0.34 (┬▒0.25) | 0.7481 | |
| Moderate (n=27)* | 0 | 5.08 (┬▒0.26) | 4.80 (┬▒0.23) | 0.242 | 5.00 (┬▒0.62) | 4.92 (┬▒0.17) | 0.8661 |
| (n=28)* | 6 | 5.70 (┬▒0.26) | 5.47 (┬▒0.23) | 0.1936* | 6.00 (┬▒0.62) | 5.55 (┬▒0.17) | 0.6669* |
| 12 | 5.75 (┬▒0.26) | 5.32 (┬▒0.44) | 0.0002* | 5.77 (┬▒0.26) | 0.0025* | ||
| 24 | 5.55 (┬▒0.58) | 4.76 (┬▒0.58) | 0.7250* | 5.17 (┬▒0.40) | 0.4392* | ||
| 0 vs. 24 | +0.46 (┬▒0.55) | -0.04 (┬▒0.56) | 0.7934 | +0.24 (┬▒0.38) | 0.7934 | ||
| Severe | 0 | ||||||
| (n=5)ŌĆĀ | 6 | ||||||
| 12 | |||||||
| 24 | |||||||
| 0 vs. 24 | |||||||
The other was p value of group comparisons at a specific time point 0, 0 vs. 24 months respectively.
* Anterior vs posterior: Patients with the same anterior and posterior hemorrhage volumes were excluded.
** Midbrain vs pontine: Patients with the same anterior and posterior hemorrhage volumes were excluded.
Table┬Ā4.
| Hemorrhage volume | Death n (%) in 24 months | HR (95% CI)* | p-value |
|---|---|---|---|
| Mild (n=61) | 20 (32.8%) | 1.00 | |
| Moderate (n=28) | 25 (89.3%) | 5.57 (2.48-12.51) | < 0.0001 |
| Severe (n=12) | 12 (100%) | 11.68 (4.12-33.16) | < 0.0001 |
| Location analysis 1 | |||
| ŌĆāAnterior | 25 (69.4%) | 1.00 | |
| ŌĆāPosterior | 24 (42.9%) | 0.35 (0.18-0.68) | 0.0020 |
| Location analysis 2 | |||
| ŌĆāMidbrain | 4 (57.1%) | 1.00 | |
| ŌĆāPontine | 45 (52.9%) | 1.52 (0.34-0.85) | 0.5867 |
HR: Hazard ratio.
Cells numbered 1ŌĆō4, 9ŌĆō12, 17ŌĆō20, and 25ŌĆō28 were classified into the anterior portion, while all other cells were placed into the posterior portion. Cells numbered 1ŌĆō16 were classified into the midbrain portion, while all others were placed into the pontine portion (Fig. 1).
* Multivariable adjusted analysis used. Adjustment factor was used, as in Table 1.
REFERENCES
- TOOLS
-
METRICS

-
- 3 Crossref
- 4,977 View
- 99 Download
- Related articles in JNIC