Intraventricular Lavage Via Bilateral Extraventricular Lavage: A Case Report and Literatures Review
Article information
Abstract
Ventriculitis has a poor prognosis, and treatment is technically challenging. We describe a case of ventriculitis in which bilateral continuous extraventricular lavage was performed and review the previously published literature on the treatment of ventriculitis using extra-ventricular drainage (EVD). A 75-year-old woman with ventriculitis and empyema was managed using an extra-ventricular drainage catheter inserted bilaterally at Kocher’s point. As the intravenous meropenem as empirical antibiotics preoperatively had been administered, the meropenem-mixed saline was continuously dripped through one EVD catheter intraoperatively. Approximately 1 L of saline with antibiotics was drained until grossly clear fluid flowed through the other EVD catheter. The follow-up MRI and the cerebrospinal fluid profile appeared to have improved. The ventriculoperitoneal shunt was performed due to secondary hydrocephalus in the course. Three months later, the patient was available for cane gait and is currently undergoing follow-up without neurological complications.
INTRODUCTION
Ventriculitis is a neurosurgical disease with a high mortality rate. The mortality rate of ventriculitis is approximately 30–71%, despite appropriate treatments1,2). In 2017, intravenous (IV) injection of antibiotics was suggested as the primary treatment by the Infectious Disease Society of America (IDSA) guidelines. If IV treatment is ineffective, antibiotic administration through intrathecal injection should be performed3). Methods of injecting antibiotics directly into the intralumbar or intraventricular space have been introduced for injecting antibiotics into the intrathecal. Invasive procedures, such as Ommaya’s reservoir or external ventriculostomy, inject drugs into the ventricle but are known to be more effective because antibiotics can be directly injected into the ventricle with a small injection amount4).
Al Menabbawy et al. introduced treatment with ventricle lavage using endoscopy, especially in children, where continuous lavage through neuro-endoscopy resulted in effective treatment and improved prognosis5). However, neuro-endoscopy has disadvantages such as lack of equipment and skilled experts and long operating time, making it less accessible than other procedures. We treated a patient with ventricular inflammation using extraventricular lavage (EVL) through bilateral Kocher's point extraventricular drainage (EVD) insertion, an easy and effective treatment method familiar to neurosurgeons. In addition, it may be an effective alternative treatment for ventriculitis.
CASE REPORT
A 75-year-old woman visited our outpatient clinic complaining of submandibular swelling and fever. She was taking medication for diabetes and hypertension; however, laboratory findings revealed that her random blood sugar was poorly controlled (555 mg/dL in the initial laboratory study). To localize the infection focus, pharynx computed tomography (CT) with enhancement revealed a submandibular abscess (Fig. 1). Extraoral incision and drainage were performed by the dentist, and ampicillin/sulbactam was administered intravenously as empirical antibiotics. However, Klebsiella pneumoniae was identified in the patient’s blood culture, and the antibiotic regimen was changed to meropenem. However, the patient had a dismal clinical course. Three days after the dental procedure, the patient showed drowsiness, aphasia, and poor cooperation. Emergent brain magnetic resonance imaging (MRI) showed enlargement of both lateral ventricles and diffusion-weighted images revealed diffusion restriction on the occipital horns of both lateral ventricles and the third ventricle (Fig. 2). The cerebrospinal fluid (CSF) profile (glucose, 1 mg/dL; protein, 1206.8 mg/dL; white blood cell, >1000/mm3; polymorphic neutrophils, 88%) suggested bacterial meningitis, and Klebsiella pneumoniae was identified in the CSF culture. For emergent CSF diversion, the patient was referred to the neurosurgery department for emergent extraventricular drainage. The EVD catheters were inserted bilaterally at Kocher’s points. Before the EVL was performed, the communication between both lateral ventricles was confirmed. The author confirmed that about 5 cc of normal saline was administered through the catheter inserted into one ventricle and a comparable amount of fluid was drained through the other ventricle without significant intracranial pressure changes.
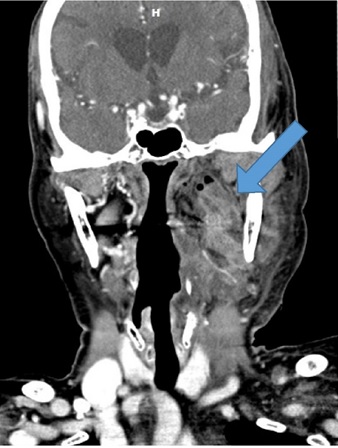
The arrow shows a submandibular abscess. The formation of abscess cavity with surrounding air bubbles are also found on computed tomography images.
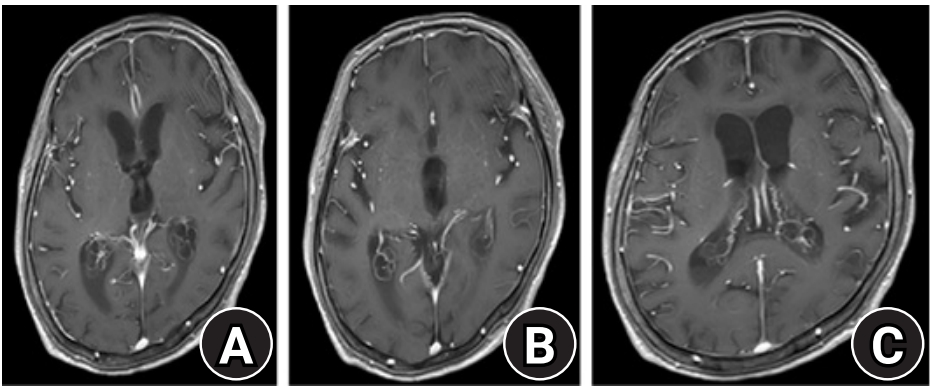
All images are taken under T1 contrast enhancement: (A) shows both ventricular walls Enhancement, (B) shows ventricular emphysema at the occipital horn, and (C) shows ventricular enlargement of the lateral ventricles.
Empirical intravenous meropenem was recommended by the physician of infectious medicine for the submandibular abscess and the ventriculitis that has spread from the submandibular abscess before confirmation of microorganisms. Thus, the author decided to keep meropenem through IV for ventriculitis and conducted lavage into the ventricle using the same antibiotic. Meropenem for EVD lavage was used by mixing 1 g of meropenem with 1 L of normal saline. Intraoperatively, saline mixed with meropenem was dripped through one catheter, and turbid fluid was drained through the other until the draining fluid became grossly clear. Serial CSF cultures after bilateral EVL did not reveal any additional bacterial strains. The CSF profile improved during hospitalization (Table 1). After removing the EVD catheter, a follow-up brain MRI revealed a consecutive increase in ventricle size, respiratory distress, decreased consciousness, and impression with secondary hydrocephalus, and for CSF diversion, an Ommaya reservoir was inserted. For 2 weeks postoperatively, meropenem IV had been continuously used, and CSF analysis after 4 weeks of EVD lavage showed an improvement (protein, 219.3.8 mg/dL; white blood cell, 15/mm3WBC) compared to the initial CSF profile (Table 1); hence, it was changed to an oral antibiotic, ciprofloxacin. The follow-up CSF profile at 1 month postoperative showed a sustained improvement (protein, 107.3 mg/dL; white blood cell, 9/mm3WBC) (Table 1). With serial improvement in CSF profile without additional infection, the ventriculoperitoneal shunt for symptomatic hydrocephalus was performed after removing the previous Ommaya’s reservoir. One month after EVL, the CSF profile showed no more evidence of infection; then, all antibiotics were discontinued (Table 1). After discharge from the hospital, on week 31 of bilateral EVL, she visited the outpatient clinic on foot, relied on a cane, and showed no significant neurological impairment.
DISCUSSION
Ventriculitis is a fatal infectious disease with a mortality of 30–70%5). Typical causes of ventriculitis include head trauma, brain abscess, meningitis, pneumonia, and post-surgical infections3). In addition, the most common strain associated with ventriculitis is coagulase-negative Staphylococcus4). In conventional treatment, the antibiotic infusion is continued to maintain an appropriate dose systemically3). To maintain a systematic antibiotic concentration, it can be injected intravenously or intraventricular.
The blood–brain barrier (BBB) is an unavoidable hurdle for intravenous antibiotics to reach the target organs in the central nervous system (CNS). Antibiotics are restricted from diffusing into the CNS due to tight junctions in the BBB, molecular size, and lipid solubility6). For example, <9% of the total intravenous injection concentration of meropenem reaches the ventricle4). However, there is no such barrier between the CSF and ventricular space; thus, antibiotics can spread relatively easily.
In ventriculitis, it is difficult to reach effective antibiotic therapeutic concentrations intravenously, and the fatality rate is high. As such, direct intrathecal injection through the intralumbar or intraventricular route is being used as an alternative to overcome the limitations of intravenous administration.
When antibiotics are administered through intralumbar routes, peak arrival time is longer than intraventricular routes, and the highest reached concentration is lower4). Therefore, if administered directly to the ventricle, the total dose of antibiotics required to reach the treatment concentration will be small; hence, side effects can be expected to be reduced.
In addition to showing improved therapeutic outcomes, endoscopic intraventricular lavage has several advantages. When antibiotics are injected directly into the intraventricular space through an endoscope, less time is required to reach the therapeutic level through fewer doses than when administered intravenously2). Additionally, it is effective in preventing the occurrence of secondary infection because the surgery is performed under more aseptic conditions5). Moreover, considering the biological aspect, there is no restriction on the passage of antibiotics through BBB; therefore, more effective antibiotic reactions can be expected6).
However, effective endoscopic interventional lavage has some limitations. An endoscopic instrument must be prepared, it takes a considerable amount of time to prepare for scrub and operation, and more decisively, the operation time is very long. Depending on the proficiency of the surgeon performing the procedure, additional complications may occur during or after the surgery.
The method of burr hole trephination through both Kocher’s points implemented in our case and placing the catheter in the ventricle can overcome the critical disadvantages of endoscopic lavage. Approaching Kocher's point is a familiar procedure for most neurosurgeons and does not require high proficiency; thus, it can be performed at the bedside in case of emergency, and no specialized instruments are required.
Moreover, there is a limitation to this method of approaching a bilateral Kocher’s point. If the catheter is attracted to the frontal horn by approaching Kocher's point and lavaged, the formation of laminar flow is relatively reduced compared to when it is maintained in the occipital horn, and the effect of the antibiotic is relatively reduced5). Furthermore, in the current case, before the lavage procedure, the CSF pathway communication was not secured and septostomy was not performed. For checking CSF pathway communication, injection of dye intraoperatively or preoperative imaging workup such as cine MRI should be conducted. Because the CSF pathway could have been blocked secondarily by inflammation and resulted to ICP elevation during lavage fluid administered. That would be safer and more reasonable to decide whether this patient can be a candidate for EVL.
CONCLUSIONS
The current case shows that ventriculitis may be treated more effectively with the method we described herein; its safety and effectiveness have been reported not only in our case but also in various other studies. More cases and long-term follow-ups are necessary to establish lavage with EVD procedure as an effective conventional administration of antibiotics option for ventriculitis.
Notes
CONFLICTS OF INTEREST
The authors declare that they have no competing interests.
