Clinical Inertia: The Care Gap between Clinical Guidelines and Clinical Practice in Neurotrauma
Article information
Traumatic brain injury is an important cause of disability, especially in the young population. According to Center for Disease Control and prevention data, there has been an increase in cases in the last 2 decades, despite the notable development of preventive technologies and the development of management guides. Clinical inertia is a concept where late initiation or lack of intensification of treatment in a patient and the failure to achieve the goals established from the beginning. This can be defined in the management term as therapeutic inertia. This concept is well known in pathologies such as hypertension and diabetes, in which we do not reach the therapeutic goal, and this carries the risk of deterioration of the patient1). It is known that therapeutic inertia occurs in half of the cases due to failures by the clinicians, in 30% associated with the patient himself, and 20% due to the characteristics of the health care system.
The burden of brain trauma injury leads to multiple Swiss cheese breakthroughs with clinical inertia is one of the unknown factors. To better understand the element of clinical inertia and traumatic brain injury management, a brief visit to the process of traumatic brain injury will be helpful. Traumatic brain injury management starts in the field, followed by a transit time to the trauma bay. In trauma bay, most of the level trauma centers already have a trauma team present to receive traumatic brain injury. Here things can get complicated. The patient needs to have 2 levels of trauma reviews including imaging studies, a neurosurgical consult, and further management. Some patients go to the operating room but mostly end up in the trauma intensive care for at least 72 hours before a major neurosurgical procedure is performed. After 72 hours, the neurocritical care management has different phases: acute phase, stabilization phase/non-survival phase, and discharge planning. All these phases lead to multiple areas of clinical inertia. This clinical inertia is related to progression of care, change of shifts, the arrival of new admits, and major disasters like the present Covid-19 pandemic. Looking at the progression of care in traumatic brain injury patients, multiple steps can be reviewed, and a stage is set to reduce the risk of clinical inertia (Fig. 1).
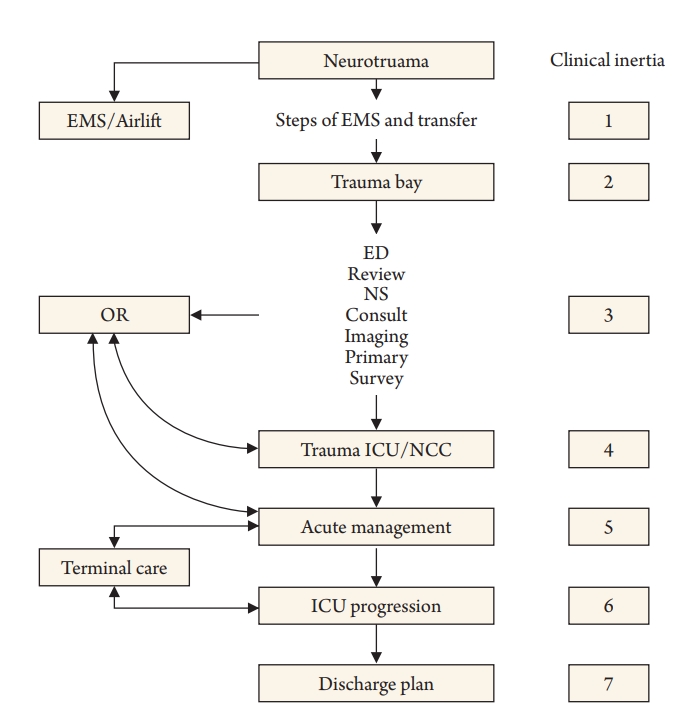
Proposed stages where clinical Inertia can play a role in the flow of the patient care with acute traumatic brain injury.
Step 1
This is the time when traumatic brain injury is first noticed in the field and emergency medical staff is called for initiation of care. There is a delay by the first responder due to trying to take steps to stabilize the injuries vs getting the victim to level 1 trauma center. The next aspect is the response of emergency medical staff, which can have multiple limitations including but not limited to other emergencies in the area and disaster situations. Emergency medical staff focuses more on the airway might lead to a delay in recognition of severe traumatic brain injury signs like unequal pupils in an awake patient. It is easy to be sidetracked due to profound hypoxemia with acute pneumothorax or an active bleeding extremity.
Step 2
Traumatic brain injury arrival to step 2 leads to activation of trauma team which includes neurosurgical evaluation. This is a crucial stage in decision making and triage of patients. It is easy with low Glasgow coma scale (GCS) to make the call to proceed to imaging and further workup. There are 2 aspects of care where clinical inertia can lead to delay in the management of the acute impending neurological crisis, i.e., when there are other pressing needs of trauma below the head and another one is high GCS on presentation. Imaging can lag in a patient with diffuse axonal injury though GCS is low while a focal collection of epidural hemorrhage may present with awake and alert status. A vigilant fast primary survey followed by imaging and close neuro examination might help to overcome this aspect of clinical inertia. Earlier consultation with neurosurgery and neurocritical care improves the odd of channeling trauma to the neurological injury pathway.
Step 3
Traumatic brain injury patients who end up going to neurosurgical interventions to have high likely have low GCS and injury pattern is at a high risk of decline. There are always certain limitations and clinicians have to watch for the inertia of any delay. Transport is the critical part of this clinical inertia. Who takes the patient to the operating room? What equipment is required? Any ongoing resuscitation is processing during the transport? A proper transport system in place can help with all these questions. The same is true if the patient is going to be admitted to the neurocritical care unit.
Step 4
Neurocritical care admission is required for most traumatic brain injury presentations. The earlier phase either from the emergency department or operating room requires the same process as presented in the emergency department. Clinical inertia can lead to a delay in the examination as the patient got stabilized in the emergency department or had a successful surgical procedure. These patients require central access, invasive arterial monitoring to keep cerebral perfusion pressure intact, and close cerebral monitoring with a multimodal catheter. With stable clinical signs, usually, the thought is to wait and see approach vs proactive preventive approach to avoid any neurological crisis like an incidental drop in mean arterial pressure, hypoxemia due to acute pulmonary injury, or progressive increase in central temperature. All these elements can lead to decline and loss in the positive momentum gained by emergency department and operating room resuscitative methods. Other patients in the intensive care unit with instability lead to clinical inertia for a new traumatic brain injury admission. It is known in the critical care arena that time of the day and week of the day play a key role in the initial care of traumatic brain injury patients. During nighttime shortage of attending level intensivists and on the weekend a limited staff presence leads can lead to clinical inertia and delayed early management.
Step 5
The first few hours in the intensive care unit for traumatic brain injury can be a dynamic process. After initial admission and stabilizing, the progression can be more predictable. The anticipation of peak swelling can be missed due to clinical inertia. To slow down the process and to create a plateau phase for cytotoxic edema is extremely important. Having stable vital signs and postoperative normal intracranial pressure can lead to a false sense of security due to clinical inertia. Once intracranial pressure starts going up due to maximum time of swelling, the management becomes more reactionary rather than preemptive. Keeping caregivers and families abreast with the pathway most of these patients take is part of the initial management. If the patient has not gone to the operating room in the beginning, usually it will be after 48 hours as per evidence that these patients do well with delayed decompression. During the first 48 hours, keep mean arterial pressure normal, temperature normal, having access like central and arterial line, prevention of stress ulceration and deep venous thrombosis, and management of other injures.
Stage 6
Critical care progression in traumatic brain injury patients is usually long and requires multiple interventions. Acute pulmonary management can cause clinical inertia with early weaning vs early tracheostomy. Tracheostomy timing is usually early after intracranial pressure stabilization if the patient cannot come off the ventilator with routine weaning process. The deep venous thrombosis risk is high in traumatic brain injury patients and early initiation of chemoprophylaxis is required once no further intervention is required. Clinical inertia will impact both of these factors. There are other less but still important critical care managements include early nutrition, skincare, stress ulcer prevention, devices integrity, and close clinical relationship with the family.
Stage 7
Discharge planning starts from admission. The clinical inertia can be due to clinical instability in the beginning followed by neuroprognosis. The second part is more cumbersome and requires time. The wishes and expectations of the patient play a key role and clinical inertia can cause a delay in decision making. Who makes the decision? Is the patient proceeding to a functional outcome vs marked disability? What is the baseline? How functional patient wants to be? All these questions are important, and ambiguity can be due to clinical inertia where one aspect is more important and others are not in the focus. Delay in exit from the intensive care can be due to placement limitation which can be due to ventilator dependency, renal support requirement or need for active rehabilitation for a patient who is awake and will get better faster.
Considering this discussion, flow-chart, and the evidence, it is important for clinicians to be aware of clinical inertia in traumatic brain injury care. There is a need for more research and training in the field of clinical inertia in critical care medicine, especially in the traumatic brain injury population. We suggested a structured education, followed by some interval reminder updates in the career of clinicians who are going to practice traumatic brain injury care.
Notes
Conflict of interest
No potential conflict of interest relevant to this article was reported.