Hypothermia for the Management of Intracranial Hypertension in Severe Brain Trauma: The Paradigm is Broken?
Article information
Worldwide, traumatic brain injury (TBI) comprises a combined incidence rate for all ages of approximately 350 per 100,000 person-years and is a leading cause of death and disability in trauma patients1,2). The presentation of TBI varies from mild alterations of consciousness to a comatose state and death3). However, despite the existence of many classification systems, the simplest includes mild, moderate, and severe TBI, in which the nature of the injury and the impact on the patient's clinical condition is considered4). In the last decade, a clear trend has been demonstrated towards deterioration in patients with severe TBI, in which the whole brain is affected precisely because of the characteristics and degree of injury. This deterioration may be associated with a loss of autoregulation due to the lack of reactivity of cerebral vascular pressure, resulting in hyperemia, interstitial edema and subsequent intracranial hypertension (ICH)5,6).
Normal intracranial pressure in adults is less than 15 mm Hg, values that remain above 20 mm Hg are considered pathological and are an indication for intensified treatment in patients with TBI7). It is important to consider that ICH can result from primary injury (hematoma expansion) or secondary damage (water accumulation, impaired autoregulation, ischemia, and contusion expansion). This is associated with high mortality rates, so multiple early, stepwise, and rescue management strategies have been proposed for its control, which is aimed at preventing secondary injury by avoiding hypotension, hypoxia and maintaining adequate cerebral perfusion pressure (CPP). Targeted treatment is essential and may include cerebrospinal fluid (CSF) drainage, use of hyperosmolar therapies, induction of hypothermia, hyperventilation, administration of barbiturates, or performance of decompressive surgery2,8).
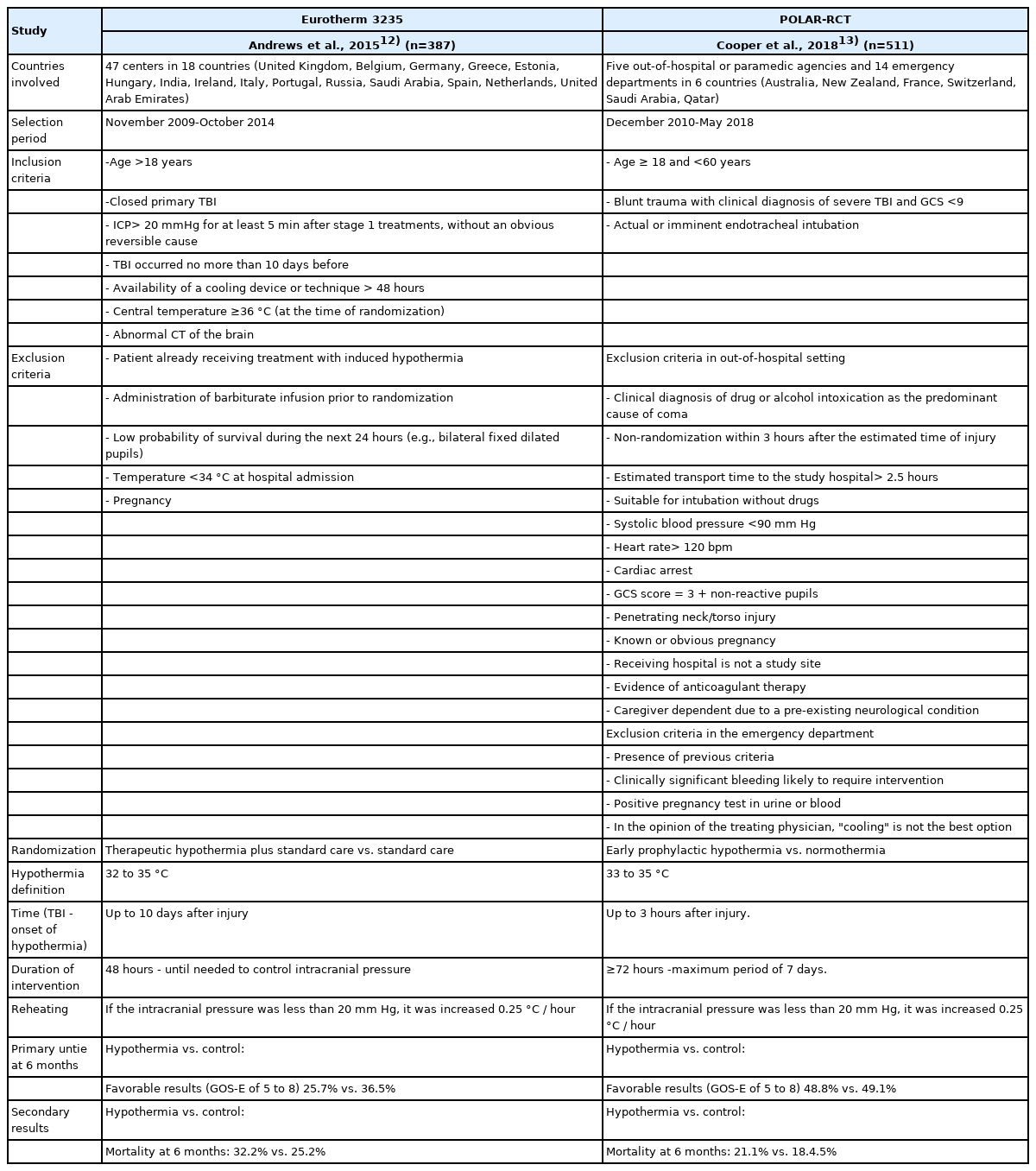
Therapeutic hypothermia (TH) is one of the few neuroprotectants that has moved from preclinical work to clinical use. For example, it was previously used to prevent brain damage during cardiac surgical procedures, but more recently it has also been used to improve both neurological and physical outcomes after sudden cardiac arrest9). Based on rodent studies, it has been found that angiogenesis and neurogenesis are stimulated by brain cooling, significantly attenuating brain infarction induced especially in the context of TBI10). Likewise, multiple analyses have led to consider TH as an attractive treatment strategy for severe TBI as it confers several theoretical benefits, including the ability to reduce ICP and increase CPP11). TH has been widely investigated as neuroprotection and treatment of ICH, however, in the setting of severe TBI it has had mixed results. Two large studies (POLAR and Eurotherm 3235) represent strong scientific evidence against its use12,13). But should it be completely discarded? Temperature changes play a critical role in neuronal vulnerability after TBI, and relatively small reductions in temperature may be effective in controlling ICH. Early therapeutic hypothermia can reduce histopathological damage by attenuating the severity of diffuse axonal injury, decreasing brain metabolism and oxygen consumption, reducing edema, stabilizing the blood-brain barrier (BBB), and promoting the survival rate in the acute stage of TBI14,15). In addition, it reduces susceptibility to post-traumatic seizures and decreases the inflammatory response to injury14). A meta-analysis reported that compared with adults who remained normothermic, those who underwent TH were associated with reduced mortality and improved neurological outcome16). However, since the central nervous system (CNS) is a complex circuit, the use of hypothermia as a management strategy may impact outcomes 6 months after the event. The Eurotherm3235 and POLAR studies have attempted to improve the available scientific evidence and constitute two major tools against the use of prophylactic and therapeutic hypothermia in patients with severe TBI, respectively (Table 1).
Eurotherm3235 evaluated the efficacy of TH plus standard care versus standard care alone and, during the first 4 days after randomization, the TH group significantly reduced elevated ICP levels, with less requirement for second or third level therapies. However, there was no significant difference in ICP in both groups on day 7 after randomization. Regarding the outcomes evaluated at 6 months, TH showed a lower percentage of favorable results and higher mortality12). There is currently controversy as to the period of hypothermia that should be used, and in this study, it may not have been long enough (>48h) to show any benefit in improving the outcome of patients with severe TBI. A recent randomized multicenter trial using a longer period of hypothermia (up to 5 days) reported a higher percentage of favorable outcomes and a lower proportion of mortality at 6 months in the intervention group (TH) compared to the normothermia group17). Although these results were not statistically significant, not all patients in the hypothermia group were able to cool to the target temperature of 34-35°C. Higher quality studies with longer TH periods may represent an important consideration for future evaluation, as some hypotheses suggest that cytotoxic edema and intracellular neurotoxicity cascades may be attenuated at the peak which is around day 5 in TBI patients11,17).
Regarding the use of TH as a rescue strategy in severe and refractory ICH, it has been very little evaluated, however, some analyses by subgroups of patients with an initial ICP ≥ 30 mm Hg, found that long-term mild TH significantly increased the favorable outcome at 6 months without raising the incidence of severe complications such as pneumonia, hypokalemia, thrombocytopenia and, arrhythmias17). Likewise, the rewarming time at Eurotherm (0.25°C /hour), which is equivalent to 3°C in only 12 hours, could have influenced the results. One analysis found that slow rewarming at a rate of <1 °C/day with a rewarming time of ≥48 hours significantly improved neurological outcomes at 6 months after mild TH in patients with severe TBI and evacuated hematoma18). So a slower rewarming period than that used in Eurotherm would form a critical element when using TH in patients with TBI
On the other hand, the POLAR-RT study did not evaluate hypothermia as a therapeutic strategy for ICH, but rather as an early prophylactic utility for TBI. This study compared prophylactic hypothermia (PH) vs. normothermia and reported good ICP control during the first 4 days post-randomization, however, is found at 6 months a lower percentage of favorable outcomes and a higher proportion of mortality in the hypothermia group13). A recently published review that included the POLAR study in its meta-analysis19) represents valuable evidence. This analysis demonstrates the importance of specific cooling parameters such as cooling temperature, cooling duration, and rewarming rate, and considers that these were a major limitation of the POLAR study, as they were only achieved in less than half of the patients who received PH, achieving a moderate level of cooling19) (Table 2).
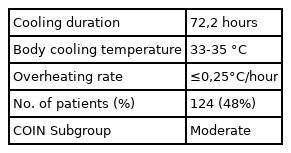
Comparison between the Eurotherm 3235 and POLAR-RCT studies regarding the use of hypothermia in the management of intracranial hypertension in traumatic brain injury
This review builds on a previous meta-analysis evaluating the effect of cooling parameters in TBI patients, which found that for trials that accurately reported the cooling protocol, there was a reduction in the odds ratio of death in the TH group compared to no cooling, concluding that TH was beneficial only if the cooling index (COIN) was sufficiently high (longer cooling and at temperature ≤ 0.25°C/h)20). Likewise, when data from the POLAR study were included in a new meta-analysis published recently, the results were similar to the previous study and indicated that the use of hypothermia significantly decreased mortality in severe TBI only in cases where COIN was high19). Thus, it is possible that the decrease in COIN masks some of the outcomes evaluated in the POLAR study (favorable PH and 6-month mortality outcomes).
Taking into account the effect of hypothermia in reducing brain metabolism, considering it in the management of ICH in patients with TBI could play an important role. A clinical trial evaluating patients with severe TBI found that inducing TH aimed at achieving a 50-60% reduction in cerebral metabolic rate significantly reduced patient mortality21). This was not considered in the Eurotherm and POLAR studies and could constitute the missing gap to evaluate the benefit of TH in patients with severe TBI and their 6-month outcomes
The Eurotherm 3225 and POLAR studies show that TH and PH control ICP, but without an impact on outcomes. This leads to the idea that TBI is a changing and very diverse entity, where ICP control is important but not sufficient to improve outcomes. It is still premature to abandon the use of TH and PH in patients with severe TBI as questions and controversies remain. An evaluation of methods to induce hypothermia, as well as of multiple combinations of treatments used in the management of ICH, is needed to determine possible synergistic effects with maximal benefits. Considering the available evidence, TH should not be considered a treatment in all patients with ICH, but in our opinion, it is a very good option in selected cases (ICH > 30 mm Hg) or as a rescue strategy In addition, to have a wider field of application for its therapeutic and prophylactic use, there is a clear need for more studies that consider prolonged mild hypothermia (>5 days), slow rewarming (<1°C/day) and adequate cooling rate (high) or establish situations that may influence mortality and medium-long term outcomes.
Notes
Conflict of interest
No potential conflict of interest relevant to this article was reported.